27 results
Emotion dysregulation in bipolar disorder compared to other mental illnesses: a systematic review and meta-analysis
- Michele De Prisco, Vincenzo Oliva, Giovanna Fico, Joaquim Radua, Iria Grande, Natalia Roberto, Gerard Anmella, Diego Hidalgo-Mazzei, Michele Fornaro, Andrea de Bartolomeis, Alessandro Serretti, Eduard Vieta, Andrea Murru
-
- Journal:
- Psychological Medicine / Volume 53 / Issue 16 / December 2023
- Published online by Cambridge University Press:
- 16 October 2023, pp. 7484-7503
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
People with bipolar disorder (BD) often present emotion dysregulation (ED), a pattern of emotional expression interfering with goal-directed behavior. ED is a transdiagnostic construct, and it is unclear whether it manifests itself similarly in other conditions, such as major depressive disorder (MDD) or borderline personality disorder (BPD), or has specific features in BD. The present systematic review and meta-analysis explored ED and adopted emotion regulation (ER) strategies in BD compared with other psychiatric conditions. PubMed/MEDLINE, EMBASE, Scopus, and PsycINFO databases were systematically searched from inception to April 28th, 2022. Studies implementing validated instruments assessing ED or ER strategies in BD and other psychiatric disorders were reviewed, and meta-analyses were conducted. Twenty-nine studies yielding multiple comparisons were included. BD was compared to MDD in 20 studies (n = 2451), to BPD in six studies (n = 1001), to attention deficit hyperactivity disorder in three studies (n = 232), to anxiety disorders in two studies (n = 320), to schizophrenia in one study (n = 223), and to post-traumatic stress disorder in one study (n = 31). BD patients did not differ from MDD patients in adopting most adaptive and maladaptive ER strategies. However, small-to-moderate differences in positive rumination and risk-taking behaviors were observed. In contrast, patients with BPD presented an overall higher degree of ED and more maladaptive ER strategies. There were insufficient data for a meta-analytic comparison with other psychiatric disorders. The present report further supports the idea that ED is a transdiagnostic construct spanning a continuum across different psychiatric disorders, outlining specific clinical features that could represent potential therapeutic targets.
Meta-analysis of the variability in the individual response to pharmacological treatments for mania in bipolar disorder
- G. Anmella, M. De Prisco, V. Oliva, M. Sanabra, L. Fortea, M. Ortuño, G. Fico, A. Murru, E. Vieta, D. Hidalgo-Mazzei, A. Solanes, J. Radua
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S84
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Many studies have investigated whether there exist predictors of good response to antimanic drugs in bipolar disorder (BD). However, these factors predict response or only indicate benign illness course.
ObjectivesTo shed some light on the topic, we tested whether the response to antimanic drugs showed any variability beyond that expected by the effects of illness course and placebo.
MethodsWe included all double-blind, placebo-controlled RCTs of oral pharmacotherapies targeting adult patients with acute bipolar mania from 1991 to 2020. The primary outcome was the variance of the improvement in manic symptoms in treated individuals compared to placebo. The effect size was the log variability ratio (logVR). We performed a random-effects meta-analysis, including assessments of heterogeneity, sensitivity/cumulative/subgroup analyses, and meta-regression.
Results42 RCTs (46 comparisons) from a total of 8,438 BD patients with acute mania (53.7% male, mean age=39.3; 5,563 treatment/2,875 control groups) were included in the analysis. Individuals in active treatment groups did not show variability in the response beyond that observed in individuals under placebo (VR=1; 95% C.I.=0.97,1.03; p-value=0.97). No heterogeneity was detected between the studies (I2=0%; tau2=0%; Q=29.21; df=45; p-value=0.97). Results were similar in the leave-one-out/cumulative/subgroup analyses. Meta-regression did not show influences by age, sample size, sex, severity of manic symptoms at baseline, or clinical features (rapid cycling, mixed or psychotic features).
ConclusionsThis meta-analysis shows no evidence of differences in the individual response to treatments. These findings suggest that the average treatment effect is a reasonable assumption for the individual BD patient with acute mania. The presented article adds evidence to the equivalent results in schizophrenia-spectrum disorders, clinical high-risk state for psychosis, and major depressive disorder, not supporting classification in responders vs. non-responders. However, these findings should be balanced with results from other fields supporting such classification.
Disclosure of InterestNone Declared
Is emotion dysregulation correlated to depressive and manic symptoms of bipolar disorder? Results from a systematic review and network meta-analysis
- V. Oliva, M. De Prisco, G. Fico, A. Murru, M. Fornaro, A. Serretti, J. Radua, E. Vieta
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S275-S276
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Emotion dysregulation (ED) is a multidimensional construct involving the lack of awareness, understanding and acceptance of emotions, a reduced access to adaptive and appropriate strategies to modulate the intensity or duration of emotional responses, and the inability to control behaviors in accordance with desired goals when experiencing negative emotions. ED is outlined in the general population and several psychiatric disorders, including bipolar disorder (BD), and influences its clinical course and management, quality of life, and daily social functioning.
ObjectivesThe objective of this systematic review was to examine the correlations between maladaptive (i.e., positive and negative rumination, negative focus, risk taking behaviors, suppression, and dampening) and adaptive (i.e., cognitive reframing, adaptive coping, and acceptance) strategies of emotion regulation (ER) and depressive and manic symptoms of BD.
MethodsWe searched the literature from inception to April 12, 2022, and included studies focusing on ER/ED assessed with a validated scale. We conducted multiple pairwise meta-analyses for correlations between ED dimension (or overall ED) and the measures of depressive and manic symptoms of BD, and separate Bayesian network meta-analyses to examine which aspects of emotion regulation were most closely associated with depressive and manic symptoms of BD. The Pearson’s r coefficients were adjusted using sample-size weights and Fisher’s r-to-z transformed was conducted.
ResultsA total of 13,826 records was identified and, after duplicate removal and title/abstract evaluation, 442 were explored at the full text. Sixteen studies were finally included. Results from pairwise meta-analyses are shown in Figure 1, results from network meta-analyses in Figure 2 and 3. Both depressive and manic BD symptomatology were found to be related to maladaptive ER strategies, with the only difference of positive rumination, associated only to manic symptoms. Negative rumination and risk-taking behaviors were the strategies more correlated to both manic and depressive symptoms, as confirmed by both pairwise metanalyses and network metanalyses. On the other hand, depressive symptomatology appeared more correlated with decreased adaptive strategies than manic symptomatology.
Image:
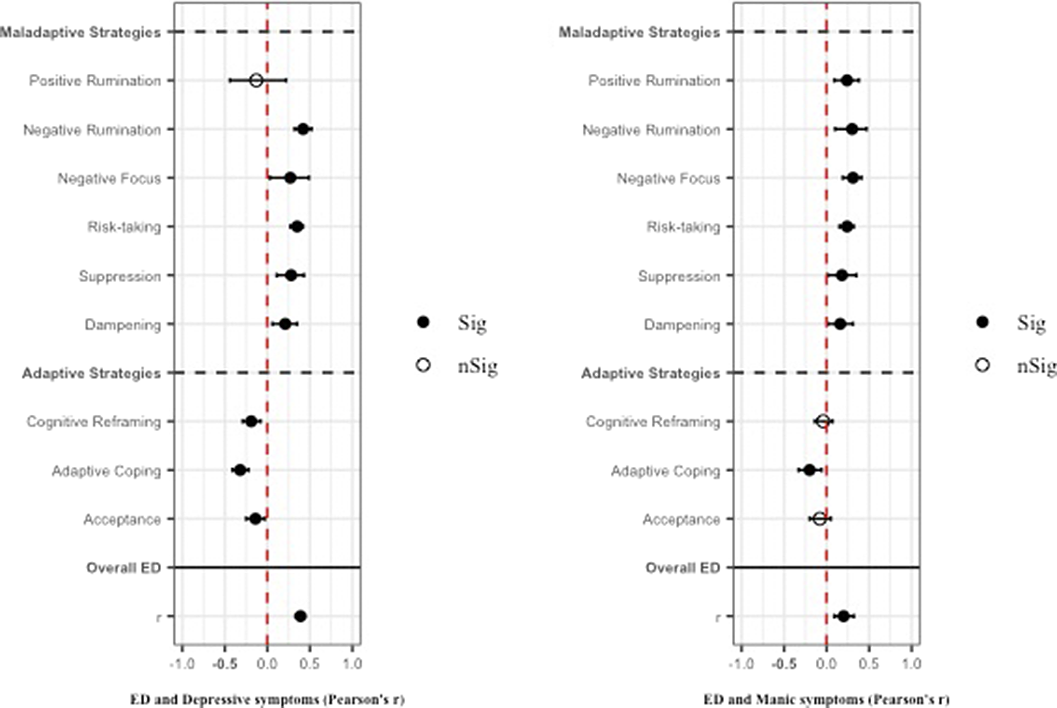
Image 2:
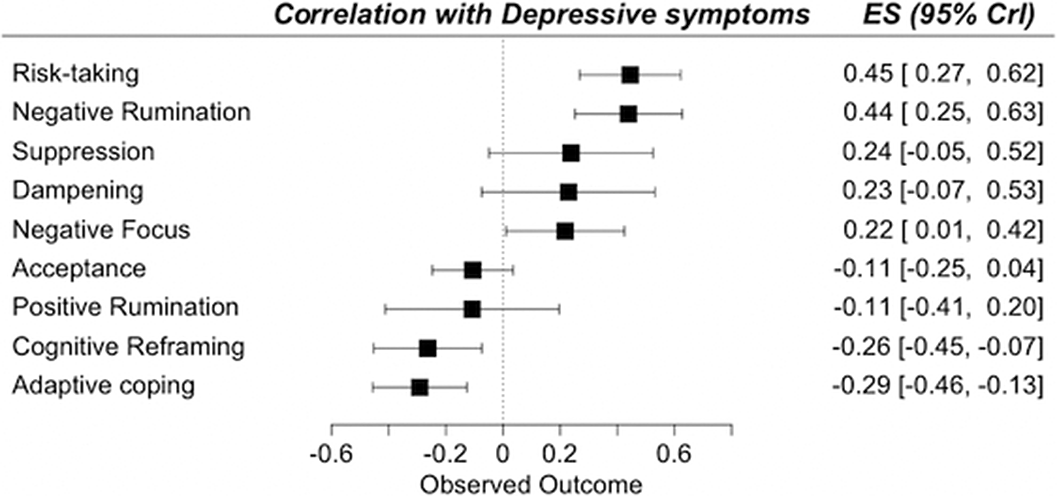
Image 3:
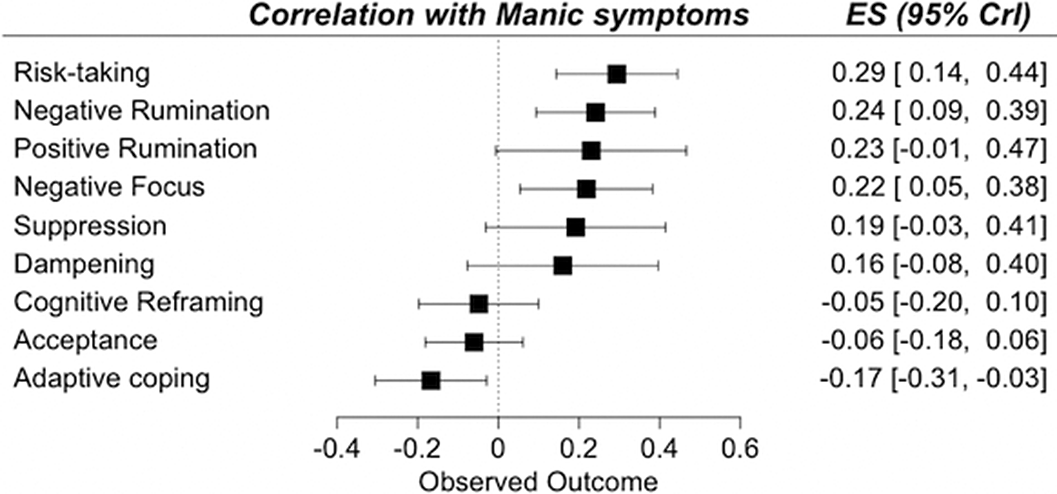 Conclusions
ConclusionsED has a significant correlation with BD symptomatology, therefore it should be explicitly considered during clinical assessment, diagnosis, and intervention on BD, and specific treatments should be implemented. More studies, and with longitudinal design, are needed to better explore these associations and their causal direction. In addition, future studies should mainly focus on the complex interactions between cognitive, social, and cultural aspects, and biological correlates to improve knowledge on a topic that is still poorly investigated.
Disclosure of InterestV. Oliva: None Declared, M. De Prisco: None Declared, G. Fico Grant / Research support from: “La Caixa” Foundation (ID 100010434 - fellowship code LCF/BQ/DR21/11880019), Consultant of: Angelini, Janssen-Cilag and Lundbeck, A. Murru Grant / Research support from: Spanish Ministry of Science and Innovation (PI19/00672) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdirección General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER), Consultant of: Angelini, Idorsia, Lundbeck, Pfizer, Takeda, M. Fornaro: None Declared, A. Serretti Consultant of: Abbott, Abbvie, Angelini, AstraZeneca, Clinical Data, Boehringer, Bristol-Myers Squibb, Eli Lilly, GlaxoSmithKline, Innovapharma, Italfarmaco, Janssen, Lundbeck, Naurex, Pfizer, Polifarma, Sanofi, Servier, and Taliaz, J. Radua Grant / Research support from: Spanish Ministry of Science and Innovation (PI19/00394, CPII19/00009) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdirección General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER) and the Instituto de Salud Carlos III, E. Vieta Grant / Research support from: Spanish Ministry of Science and Innovation (PI18/00805, PI21/00787) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdirección General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER); the Instituto de Salud Carlos III; the CIBER of Mental Health (CIBERSAM); the Secretaria d’Universitats i Recerca del Departament d’Economia i Coneixement (2017 SGR 1365), the CERCA Programme, and the Departament de Salut de la Generalitat de Catalunya for the PERIS grant SLT006/17/00357. Thanks the support of the European Union Horizon 2020 research and innovation program (EU.3.1.1. Understanding health, wellbeing and disease: Grant No 754907 and EU.3.1.3. Treating and managing disease: Grant No 945151), Consultant of: AB-Biotics, AbbVie, Angelini, Biogen, Boehringer-Ingelheim, Celon Pharma, Dainippon Sumitomo Pharma, Ethypharm, Ferrer, Gedeon Richter, GH Research, Glaxo-Smith Kline, Janssen, Lundbeck, Medincell, Novartis, Orion Corporation, Organon, Otsuka, Rovi, Sage, Sanofi-Aventis, Sunovion, Takeda, and Viatris
Does bipolar disorder differ from other mental illnesses in terms of emotion dysregulation? A systematic review and meta-analysis
- M. De Prisco, V. Oliva, G. Fico, J. Radua, I. Grande, N. Roberto, G. Anmella, D. Hidalgo-Mazzei, M. Fornaro, A. de Bartolomeis, A. Serretti, E. Vieta, A. Murru
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S571-S572
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Emotion regulation (ER) is the ability to assess, monitor, or modify emotional reactions to achieve a goal (Gross. Psychological inquiry 2015; 26 1-26). When ER strategies are rigidly or maladaptively applied, emotional dysregulation (ED) can occur (Thompson. Development and psychopathology 2019; 31 805-815). ED is common in people diagnosed with bipolar disorder (BD), but it can also be described in other clinical populations given its transdiagnostic nature. Numerous aspects of ED have been described in BD (De Prisco et al. Neuroscience & Biobehavioral Reviews 2022; 104914), but it is unclear whether these manifest similarly in other conditions such as major depressive disorder (MDD) or borderline personality disorder (BPD), or whether they are specific to BD.
ObjectivesThe objective of this systematic review and meta-analysis is to examine the literature comparing BD with other psychiatric disorders in terms of ED, focusing on those studies using validated clinical tools.
MethodsA systematic search from inception to April 28th, 2022, was conducted exploring the PubMed/MEDLINE,EMBASE, Scopus, and PsycINFO databases. Those studies providing quantitative data on ED in people diagnosed with BD and compared with clinical groups were eligible for inclusion. No restriction about age, sample size, or language were applied. Random effect meta-analyses were conducted, and effect sizes were calculated as standardized mean differences (SMD).
ResultsA total of 3,239 records was identified and, after duplicate removal and title/abstract evaluation, 112 were explored at the full text. Twenty-nine studies were finally included, and it was possible to perform a meta-analysis with twenty-two (145 comparisons) of them. Only studies comparing BD with MDD, and BPD provided sufficient data to perform a meta-analysis. People with BD did not differ from people with MDD in most of the comparisons considered. However, BD patients presented higher positive rumination (two comparisons: SMD=0.46; CI=0.27, 0.64; p=8.5e-07; I2=0%; and SMD=0.34; CI=0.15, 0.52; p=2.7e-04; I2=0%) and risk-taking behaviors (SMD=0.48; CI=0.27, 0.69; p=8.11e-06; I2=0%). In contrast, people with BPD displayed an overall higher degree of ED (SMD=-1.22; CI=-1.94, -0.5; p=9.1e-04; I2= 90.7) and used fewer adaptive ER strategies. Additionally, higher levels of self-blaming (SMD=-0.80; CI=-1.11, -0.50; p=2.68e-07; I2=0) and impulsive behavior (SMD=-0.76; CI=-0.89, -0.63; p=5.4e-29; I2=0) were observed.
Image:
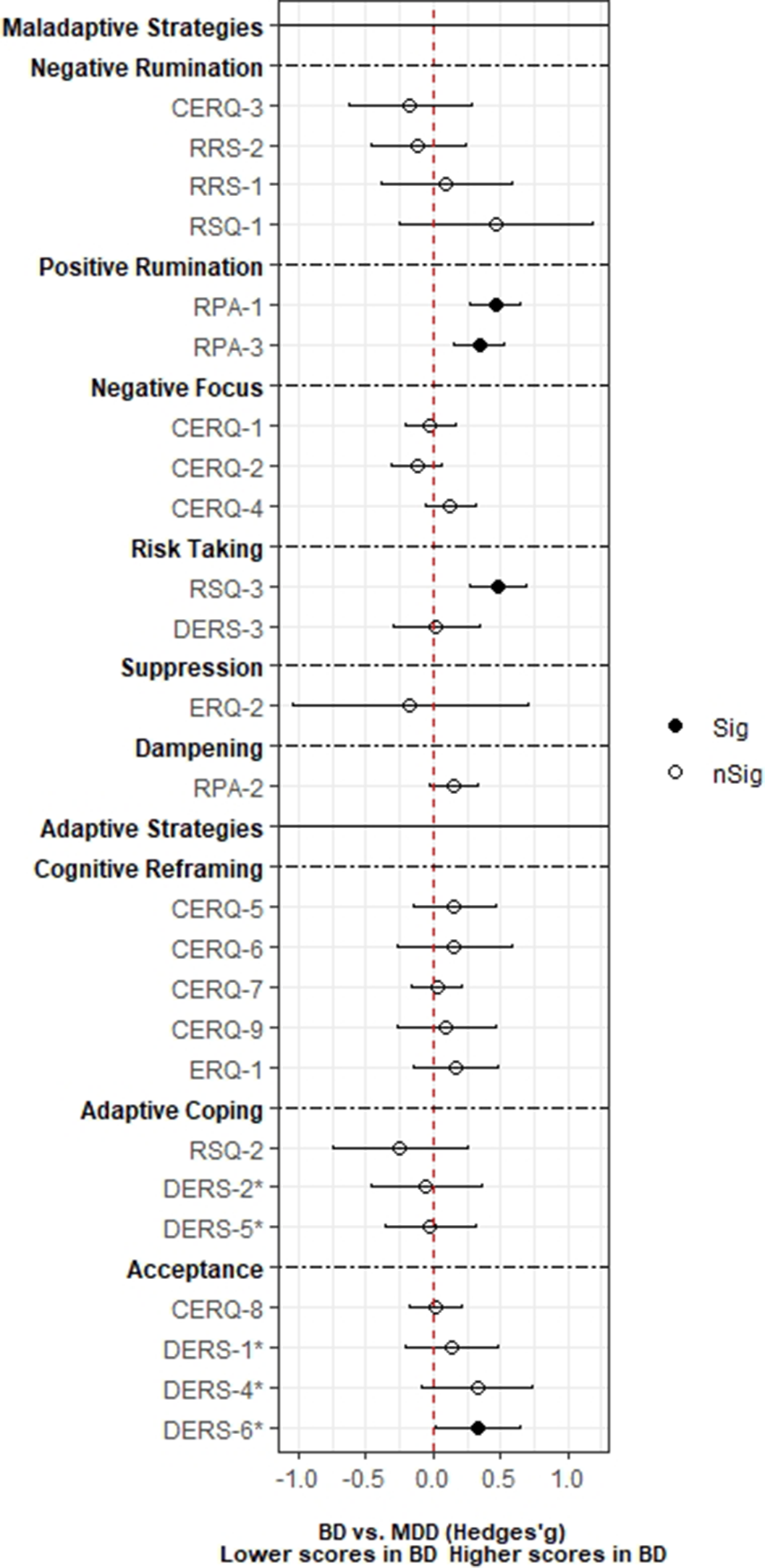
Image 2:
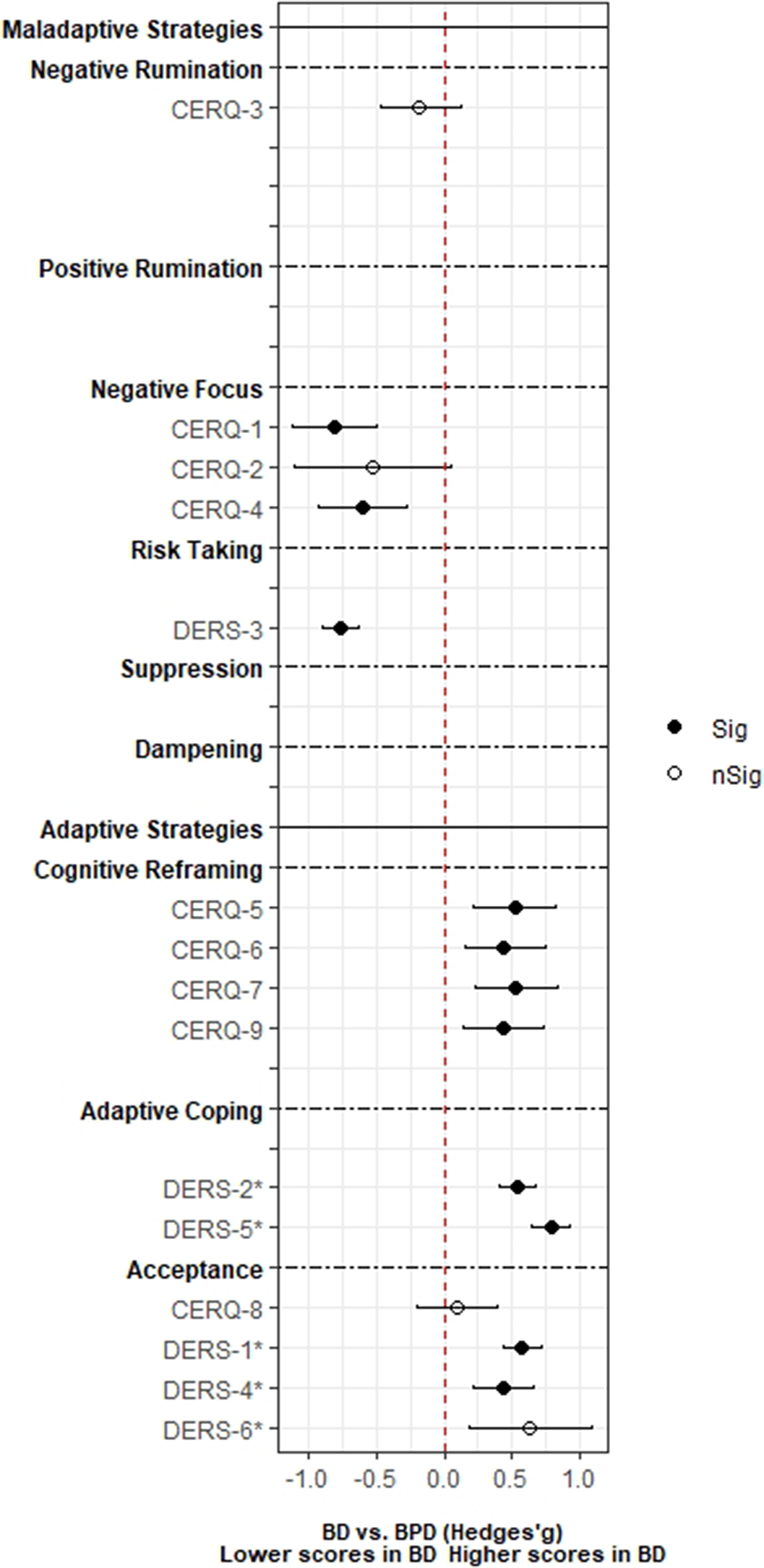 Conclusions
ConclusionsED is a trans-diagnostic construct that spans a continuum of different psychiatric disorders. Outlining the specific clinical features of one disorder versus another may help future research to increase our knowledge of these issues and develop new treatment strategies to reduce the clinical burden of these patients.
Disclosure of InterestM. De Prisco: None Declared, V. Oliva: None Declared, G. Fico Grant / Research support from: “La Caixa” Foundation (ID 100010434 - fellowship code LCF/BQ/DR21/11880019), Consultant of: Angelini, Janssen-Cilag and Lundbeck, J. Radua Grant / Research support from: Spanish Ministry of Science and Innovation (PI19/00394, CPII19/00009) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdirección General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER) and the Instituto de Salud Carlos III, I. Grande Grant / Research support from: Spanish Ministry of Science and Innovation (MCIN) (PI19/00954) integrated into the Plan Nacional de I+D+I and cofinanced by the ISCIII-Subdirección General de Evaluación y el Fondos Europeos de la Unión Europea (FEDER, FSE, Next Generation EU/Plan de Recuperación Transformación y Resiliencia_PRTR ); the Instituto de Salud Carlos III; the CIBER of Mental Health (CIBERSAM); and the the Secretaria d’Universitats i Recerca del Departament d’Economia i Coneixement (2017 SGR 1365), CERCA Programme / Generalitat de Catalunya as well as the Fundació Clínic per la Recerca Biomèdica (Pons Bartran 2022-FRCB_PB1_2022), Consultant of: ADAMED, Angelini, Casen Recordati, Ferrer, Janssen Cilag, and Lundbeck, Lundbeck-Otsuka, Luye, SEI Healthcare, N. Roberto: None Declared, G. Anmella Grant / Research support from: Rio Hortega 2021 grant (CM21/00017) from the Spanish Ministry of Health financed by the Instituto de Salud Carlos III (ISCIII) and co-financed by the Fondo Social Europeo Plus (FSE+), Consultant of: Janssen-Cilag, Lundbeck, Lundbeck/Otsuka, and Angelini, D. Hidalgo-Mazzei Grant / Research support from: Juan Rodés JR18/00021 granted by the Instituto de Salud Carlos III (ISCIII), M. Fornaro: None Declared, A. de Bartolomeis Consultant of: Janssen, Lundbeck, and Otsuka and lecture fees for educational meeting from Chiesi, Lundbeck, Roche, Sunovion, Vitria, Recordati, Angelini and Takeda; he has served on advisory boards for Eli Lilly, Jansen, Lundbeck, Otsuka, Roche, and Takeda, Chiesi, Recordati, Angelini, Vitria, A. Serretti Consultant of: Abbott, Abbvie, Angelini, AstraZeneca, Clinical Data, Boehringer, Bristol-Myers Squibb, Eli Lilly, GlaxoSmithKline, Innovapharma, Italfarmaco, Janssen, Lundbeck, Naurex, Pfizer, Polifarma, Sanofi, Servier, and Taliaz, E. Vieta Grant / Research support from: Spanish Ministry of Science and Innovation (PI18/00805, PI21/00787) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdirección General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER); the Instituto de Salud Carlos III; the CIBER of Mental Health (CIBERSAM); the Secretaria d’Universitats i Recerca del Departament d’Economia i Coneixement (2017 SGR 1365), the CERCA Programme, and the Departament de Salut de la Generalitat de Catalunya for the PERIS grant SLT006/17/00357. Thanks the support of the European Union Horizon 2020 research and innovation program (EU.3.1.1. Understanding health, wellbeing and disease: Grant No 754907 and EU.3.1.3. Treating and managing disease: Grant No 945151), Consultant of: AB-Biotics, AbbVie, Angelini, Biogen, Boehringer-Ingelheim, Celon Pharma, Dainippon Sumitomo Pharma, Ethypharm, Ferrer, Gedeon Richter, GH Research, Glaxo-Smith Kline, Janssen, Lundbeck, Medincell, Novartis, Orion Corporation, Organon, Otsuka, Rovi, Sage, Sanofi-Aventis, Sunovion, Takeda, and Viatris, A. Murru Grant / Research support from: Spanish Ministry of Science and Innovation (PI19/00672) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdirección General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER), Consultant of: Angelini, Idorsia, Lundbeck, Pfizer, Takeda
A family history of suicide in bipolar disorders: powerful, powerless
- M. Sagué Vilavella, G. Fico, G. Anmella, A. Giménez, M. Gómez Ramiro, M. T. Pons Cabrera, S. Madero, A. Murru, E. Vieta
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S387
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
When completing the medical record of a patient with bipolar disoder (BD), hardly anything is more impacting than a family history of completed suicide (FHS). In fact, FHS is a main risk factor for personal suicide attempts and death in this population. There are few modifiable protective factors against suicide in BD, such as lithium treatment and absence of substance abuse.
ObjectivesWe aimed to explore the relationship between a FHS and clinical characteristics in patients with BD. Given the impact that FHS has on the individual and on healthcare professionals, we hypothesized that it would modify behaviors towards a higher prevalence of the modifiable protective factors against suicide, namely more treatment with lithium and less drug addiction.
MethodsThis is a cross-sectional study that included all patients with BD that were followed up in a specialised unit between 1998 and 2020. Only subjects with complete information on FHS were retained for the analysis. We assessed sociodemographic and clinical data and described it with measures of frequency, central tendency and dispersion. Differences between subjects with and without FHS were calculated with χ², Fisher’s exact test and Student’s t-test as appropriate. We set the significance level at p≤0.05. All tests were two-tailed.
ResultsThe sample consisted of 480 subjects with a mean age of 45.9 years (standard deviation 14.4, range 18-88), of which 54.4% (n=261) were women. 69.2% (n=332) had a diagnosis of BD type I and 30.8% (n=148) of BD type II. 77 subjects (16%) had a FHS. Regarding differences between groups, those with relatives who had committed suicide did not show statistically significant differences in terms of sociodemographic variables (age, gender, civil status, employment) or key clinical features (type of BD, illness duration, psychotic features, predominant polarity, rapid cycling, number of lifetime manic and depressive episodes, comorbid personality disorder), neither did they have a higher use of lithium (55.8% vs 59.3%, p=0.572) nor lower substance use disorder (10.9% vs 15.5%, p=0.34). Predictably, people with FHS had a higher prevalence of family history of mental and affective disorders (96.1% vs 70.9%, p<0.001; 86.3% vs 56.3%, p<0.001) and of stressful life events (71.6% vs 58.9%, p=0.05). Personal lifetime suicide attempts also tended to be higher (36.4% vs 26.7%, p=0.088).
ConclusionsContrary to our hypothesis, in our sample of subjects with BD a FHS was not associated with a higher prevalence of the modifiable protective factors against suicide. Therefore, although suicide has a major impact both in families and healthcare professionals, our results suggest it does not modify attitudes towards prevention in a real-life scenario. The main limitation of our study is its cross-sectional design, which does not allow for causal inference. In conclusion, there is room for improvement in the fight against suicide.
Disclosure of InterestNone Declared
Lifetime number of affective episodes and functioning in a cohort of patients with bipolar disorder: A cross-sectional study
- L. Colomer, G. Fico, F. Gutiérrez, E. Pujal, N. Baldaquí, A. Murru, E. Vieta
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S384
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Cognitive impairment has been commonly found in patients with bipolar disorder (BD).(1) Recent evidence supports the view that global and cognitive functioning decrease as a function of number of prior mood episodes, but the relationship is still not clear. (2)
ObjectivesWe conducted a cross-sectional study to explore the associations between the lifetime number of affective episodes and functioning, in particular, cognitive functioning in a cohort of patients with BD.
MethodsAdult patients with BD were recruited if euthymic for at least 3 months. Socio-demographic and clinical variables were recollected at the baseline evaluation. Functioning was evaluated at baseline with the functioning assessment short test (FAST). The strength of the association between the lifetime number of affective episodes and FAST subscores was explored with Spearman’s correlation test. Linear regression was computed using cognitive functioning as the dependent variable and a set of clinically relevant variables including the lifetime number of affective episodes as independent variables after controlling for illness duration.
Results261 BD patients were recruited. Patients with a higher number of lifetime affective episodes showed a significant positive correlation with higher FAST global score (r=0.334, p<0.001) and FAST cognitive functioning subscore (r=0.331, p<0.001). At the linear regression, a higher number of affective episodes was associated to worse cognitive functioning (b=0.037, 95%CI [0.011-0.064], p=0.005).
ConclusionsPoor cognitive functioning in BD could be the result of multiple affective relapses. A timely diagnosis with subsequent effective prophylactic treatment may prevent poor functional outcomes in real-world patients with BD.
Disclosure of InterestNone Declared
The Blackshirts’ Dictatorship: Armed Squads, Political Violence, and the Consolidation of Mussolini's Regime by Matteo Millan, translated by Sergio Knipe, London and New York, Routledge, 2022, xi + 247 pp., £130.00 (hardback), ISBN 978-1-03-222446-6.
- Alberto Murru
-
- Journal:
- Modern Italy / Volume 29 / Issue 1 / February 2024
- Published online by Cambridge University Press:
- 03 July 2023, pp. 117-118
- Print publication:
- February 2024
-
- Article
- Export citation
Psychotropic drug repurposing for COVID-19: a systematic review
- U. Isayeva, G. Fico, S. Gomes-Da-Costa, M. Sagué Villavella, A. Gimenez, M. Manchia, A. Murru
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S337
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Recently, several antidepressants, mood stabilizers, and antipsychotics have been suggested to have favorable effects in the treatment of COVID-19.
ObjectivesThe aim of this systematic review was to collect evidence from preclinical and clinical studies concerning the scientific evidence for the repurposing of psychotropic drugs in COVID-19 treatment.
MethodsTwo independent authors searched PubMed-MEDLINE, Scopus, PsycInfo, Clinical Trial Registration Site US (ClinicalTrials.gov) databases, and reviewed the reference lists of articles for eligible articles published up to May 31st, 2021. All preclinical and clinical studies on the effect of any psychotropic drug on Sars-CoV-2 or patients with COVID-19 were included. The Newcastle-Ottawa scale was used for the quality assessment of clinical studies. This systematic review adheres to the PRISMA guidelines.
Results22 studies were included in the synthesis: 9 clinical studies, 9 preclinical studies, and 4 computational studies. The use of antidepressants, both SSRI and non-SSRI, was associated with a reduced risk of severe complications of COVID-19. Several antipsychotics showed an increased risk for both Sars-CoV-2 infection and severe complications during COVID-19.
ConclusionsThe current evidence supports a potential anti-SARS-CoV-2 role for several antidepressants, while the evidence on mood stabilizers or antipsychotics remains controversial. Drug repurposing proved highly successful in response to the current pandemic and psychotropic medications are widely used in clinical practice with well-known safety and tolerability profiles, showing antiviral, immunomodulatory, and anti-inflammatory properties, being perfect candidates for possible treatment of COVID-19. Further research will deliver optimized and specific therapeutic tools that will increase the preparedness of health systems for possible future epidemics.
DisclosureNo significant relationships.
The TIMEBASE Study: IdenTifying dIgital bioMarkers of illnEss activity in BipolAr diSordEr. Preliminary results
- G. Anmella, A. Mas, I. Pacchiarotti, T. Fernández, A. Bastidas, I. Agasi, M. Garriga, N. Verdolini, N. Arbelo, D. Nicolás, V. Ruiz, M. Valentí, A. Murru, E. Vieta, A. Solanes, F. Corponi, B. Li, D. Hidalgo-Mazzei
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S221
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Mood episodes in bipolar disorder (BD) are still identified with subjective retrospective reports and scales. Digital biomarkers, such as actigraphy, heart rate variability, or ElectroDermal activity (EDA) have demonstrated their potential to objectively capture illness activity.
ObjectivesTo identify physiological digital signatures of illness activity during acute episodes of BD compared to euthymia and healthy controls (HC) using a novel wearable device (Empatica´s E4).
MethodsA pragmatic exploratory study. The sample will include 3 independent groups totalizing 60 individuals: 36 BD inpatients admitted due to severe acute episodes of mania (N=12), depression (N=12), and mixed features (N=12), will wear the E4-device at four timepoints: the acute phase (T0), treatment response (T1), symptoms remission (T2) and during euthymia (T3; outpatient follow-up). 12 BD euthymic outpatients and 12 HC will be asked to wear the E4-device once. Data pre-processing included average downsampling, channel time-alignment in 2D segments, 3D-array stacking of segments, and random shuffling for training/validation sets. Finally, machine learning algorithms will be applied.
ResultsA total of 10 patients and 5 HC have been recruited so far. The preliminary results follow the first differences between the physiological digital biomarkers between manic and depressive episodes. 3 fully connected layers with 32 hidden units, ectified linear activation function (ReLU) activation, 25% dropout rate, significantly differentiated a manic from a depressive episode at different timepoints (T0, T1, T2).
ConclusionsNew wearables technologies might provide objective decision-support parameters based on digital signatures of symptoms that would allow tailored treatments and early identification of symptoms.
DisclosureNo significant relationships.
Bipolar disorders and suicide: stumbling twice with the same stone?
- M. Sagué-Vilavella, G. Fico, G. Anmella, A. Giménez-Palomo, M. Gómez-Ramiro, M. Pons Cabrera, S. Madero, E. Vieta, A. Murru
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S222-S223
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Suicide is the most terrible outcome of bipolar disorders (BD). It impacts families and healthcare professionals deeply. Family history of suicide (FHS) is one of its main risk factors, whereas lithium treatment and absence of substance use disorders (SUD) are two of its few modifiable protective factors.
ObjectivesTo explore the relationship between FHS and clinical characteristics in BD. We hypothesized that FHS would be associated with less SUD, higher rates of lithium treatment and shorter duration of untreated illness (DUI).
MethodsCross-sectional analysis of subjects with BD followed-up in a specialised outpatient unit (Barcelona, October’08-March’18). We described data with measures of frequency, central tendency and dispersion, and we used χ², Fisher’s test and t-tests for comparisons.
ResultsThe sample consisted of 83 subjects, 56.6% males, mean age 41.9 years (SD 12.7). 74.7% (n=62) had a diagnosis of BD-I and 25.3% (n=21) of BD-II. 11 subjects (13.3%) had FHS. Those with FHS did not show significant differences in sociodemographic data, DUI (58.5+/-60.4 vs 38.19+/-84.9 months, p=0.341), lithium use (72.7% vs 73.6%, p=0.95) or SUD (27.3% vs 23.6%, p=0.79). There were differences in terms of lifetime suicide attempts (54.5% vs 20.8%, p=0.026), family history of mental disorders (100% vs 69.4%, n=0.032).
ConclusionsContrary to our hypothesis, FHS was not associated with the modifiable protective factors against suicide (namely, less SUD and more lithium prescription). Similarly, we did not find an association with earlier access to mental health services at symptom onset (DUP as proxy). Therefore, our results suggest FHS does not modify attitudes towards prevention.
DisclosureNo significant relationships.
Dhat syndrome: A case report on a culture-bound challenge
- L. Ilzarbe, D. Ilzarbe, N. Arbelo, C. Llach, G. Anmella, E. Vieta, A. Murru
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S733
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Dhat Syndrome is a culture-bound entity frequent in the Indian subcontinent. It is characterized by somatic symptoms, together with depressive and anxiety features, specifically focused on the belief of losing semen through urine1.
ObjectivesTo describe an atypical Dhat Syndrome case in European cultural context,and to determine the appropriate diagnostic frame and subsequent therapeutic approach.
MethodsWe present the case of a 37-year-old Indian man attended in our psychiatric outpatient unit mainly due to somatic complaints (gastrointestinal, sexual dysfunction, weakness, and dizziness). He interpreted his problem as possibly due to diabetes and hypothyroidism, and specifically from sugar loss in urine. Organic diseases were excluded.
ResultsAlthough considered as culture-bound, Dhat syndrome has been classified as a subtype of depression, anxiety disorder, somatoform disorder2,3,4, and even a prodromal phase of schizophrenia5. Antidepressants and benzodiazepines are the most recommended pharmacological treatments1. Antipsychotic agents have been used when clear psychotic symptoms were present (auditory hallucinations,delusions)5. Nonetheless, paliperidone 6mg/d was initiated at baseline, with good response and partial remission of the symptoms at two weeks, despite the absence of clear psychotic features. Culturally-informed cognitive-behavioural therapy, as well as sexual education could be beneficial were planned and initiated1.
ConclusionsData on Dhat Syndrome is scarce, yet agreement exist in considering the cultural context of the patient to avoid diagnostic delays. The adequate treatment remains uncertain. Antipsychotics may be a potential treatment. Further research is necessary to clarify the nature of this syndrome but European clinicians must be aware of culturally-mediated psychiatric manifestations which are increasingly prevalent due to globalization.
DisclosureNo significant relationships.
When should mood stabilizers be withdrawn due to lack of efficacy? Some methodological considerations
- A. Murru, F. Colom, A. Nivoli, I. Pacchiarotti, M. Valenti, E. Vieta
-
- Journal:
- European Psychiatry / Volume 26 / Issue 3 / April 2011
- Published online by Cambridge University Press:
- 16 April 2020, pp. 183-186
-
- Article
- Export citation
-
Maintenance therapy in bipolar disorder is primarily aimed at preventing recurrence of acute episodes. Clinicians often decide on the basis of their own experience whether mood stabilizer (MS) is properly satisfying the objective of preventing a relapse/recurrence. Evidence-based data seem far from clinical practice in assessing a MS efficacy, as they mainly focus on a drug's efficacy to first relapse and not considering the patient's course of illness. The problem of assessing MS's efficacy seems further complicated when considering combination therapy, which, due to lack of evidence-based data, economical aspects, attitude of clinicians and legal issues may bring to cumulative prescriptions. Nowadays, the drug therapy for a bipolar patient is usually tailored after longitudinal observation of his specific course of illness. The course of illness should be considered also when choosing practical criteria for the suspension of a MS due to lack of efficacy. The authors propose some preliminary criteria which may help clinicians evaluating whether a mood stabilizer is being useful or not, dividing possible outcomes and suggesting subsequent therapeutic steps in the optimization of a patient's treatment.
Treatment non-adherence amongst schizoaffective bipolar patients: An unsolved question
- A. Murru, C.M. Bonnin, A.M. Nivoli, I. Pacchiarotti, E. Vieta, F. Colom
-
- Journal:
- European Psychiatry / Volume 26 / Issue S2 / March 2011
- Published online by Cambridge University Press:
- 16 April 2020, p. 235
-
- Article
-
- You have access Access
- Export citation
-
Introduction
Non adherence to treatment is especially common in patients with chronic relapsing disorders. Schizoaffective disorder is a chronic, severe and disabling illness consisting of the concurrent presentation of symptoms of schizophrenia and affective disorders. Its course and prognosis has been found to be intermediate to those two conditions.
ObjectivesTo evaluate treatment adherence in a schizoaffective sample and to which demographical and clinical variables it may be associated.
MethodsAdherence to treatment and its clinical correlates were assessed in 69 patients meeting DSM-IV-TR diagnosis of schizoaffective disorder, bipolar type, by means of adherence-focused interviews, measurements of plasma concentrations of mood stabilizers.
Adherent and poorly adherent patients were compared with respect to several clinical and treatment variables.
ResultsPoorly adherent patients were 40% of the total sample. Demographic variables (i.e.: gender, marital status, cultural level, employment) were not associated to treatment adherence, nor were clinical variables (age at onset, polarity of the first episode, lifetime history of seasonal pattern, rapid cycling, atypical depression, melancholia, catatonia) or family history for generic psychiatric, affective disorders and suicide. No pharmacological treatment (atypical antipsychotic, mood stabilizer and antidepressant) was associated to adherence in our sample.
ConclusionsClinical and demographical factors are not related to medication adherence in our sample. Coherently with the general severity of this condition, and since there does not seem to be any clinical predictor of poor adherence, in clinical practice all schizoaffective patients should be monitored and treated as potentially non-adherent.
Asenapine in the Treatment of Bipolar Disorder: New Insights From the Expasen Study
- D. Hidalgo-Mazzei, A. Murru, J. Undurraga, M. Reinares, A. González-Pinto, C. De Dios, J.M. Montes, E. Vieta
-
- Journal:
- European Psychiatry / Volume 30 / Issue S1 / March 2015
- Published online by Cambridge University Press:
- 15 April 2020, p. 1
-
- Article
-
- You have access Access
- Export citation
-
Introduction
Bipolar disorder is characterized by relapsing and remitting mood phases, such as manic or depressive episodes as well as periods of subsyndromal symptoms. Among the treatment options for acute manic episodes, most antipsychotics have a good level of evidence of effectiveness [1]. Asenapine is a new atypical antipsychotic which showed good effectiveness and tolerability [2] along with a reasonable cost-effectiveness [3] in placebo-controlled trials. However, few studies have tested this in real-world clinical settings so far.
ObjectiveThe aim of this study was to evaluate the effectiveness and tolerability of asenapine in bipolar patients in a naturalistic clinical setting.
MethodsWe retrospectively examined the clinical records of 94 systematically followed-up adult patients who received asenapine in four selected Spanish reference centers. We assessed sociodemographic variables, tolerability as well as clinical severity through routinely used evaluation scales.
ResultsHalf of the patients reported at least one adverse effect related to the asenapine (51%), being somnolence the most frequent (30%). Although none of the side effects reported was a cause to discontinue it. Asenapine showed good levels of effectiveness with a 61% reduction of manic and 44% of the depressive symptoms. Concerning mixed states, there was reduction of 30% and 39%, for both manic and depressive symptoms respectively.
ConclusionsThough asenapine has an indication for acute manic episodes in bipolar disorder, the present study suggests that it can also have a role in treating depressive and mixed states in a real world setting. In addition, tolerability was consistent with clinical trial data.
Signs and Symptoms Self-monitoring and Psychoeducation in Bipolar Patients with a Smart-phone Application (SIMPLe) Project
- D. Hidalgo-Mazzei, M. Reinares, A. Murru, C.M. Bonnin, E. Vieta, F. Colom
-
- Journal:
- European Psychiatry / Volume 30 / Issue S1 / March 2015
- Published online by Cambridge University Press:
- 15 April 2020, p. 1
-
- Article
-
- You have access Access
- Export citation
-
Introduction
Bipolar disorder is a frequent condition in the general population with a high morbimortality, which consists in dysfunctional temporal fluctuations between different mood phases during which frequently there is a lack of insight. Besides the pharmacological treatment, psychoeducational programs have proved to be a cost-effective approach to help patients recognize early signs and symptoms in order to prevent full-blown episodes, although its broad implementation is still difficult and costly [1].
Objectives and AimsThe main aim of this study is to develop and clinically validate a smartphone application to monitor symptoms and signs in stable bipolar patients along with customized embedded psycho-education contents and empower the self-management of their disorder to avoid relapses and hospitalizations.
MethodsThe study will be carried out in three different but complementary phases in order to fully include patients and therapist's preferences: 1. Feasibility study using SIMPLe 1.0 app (subjective information only). 2. Feedback-based improvement process which will incorporate the objective information. 3. Randomized controlled trial with two arms of 74 patients each (SIMPLe 2.0+TAU vs. TAU).
ResultsAfter the collaborative development of clinical algorithms to ensure adequate sensibility and specificity to detect relapses and personalize psychoeducational messages, a technical pilot test of SIMPLE 1.0 app is underway and the first patients are being recruited to start the 1st phase of the study in Mid-October of 2014.
ConclusionsThe possibility to deliver personalized psychoeducation contents based on monitoring signs and symptoms through a smartphone seems a promising cost-effective method, although a clinical validation is necessary.
The aggressor at the mirror: Psychiatric correlates of deliberate self-harm in male prison inmates
- N. Verdolini, A. Murru, L. Attademo, R. Garinella, I. Pacchiarotti, C. del Mar Bonnin, L. Samalin, L. Pauselli, M. Piselli, A. Tamantini, R. Quartesan, A.F. Carvalho, E. Vieta, A. Tortorella
-
- Journal:
- European Psychiatry / Volume 44 / July 2017
- Published online by Cambridge University Press:
- 23 March 2020, pp. 153-160
-
- Article
- Export citation
-
Background:
Deliberate self-harm (DSH) causes important concern in prison inmates as it worsens morbidity and increases the risk for suicide. The aim of the present study is to investigate the prevalence and correlates of DSH in a large sample of male prisoners.
Methods:A cross-sectional study evaluated male prisoners aged 18+ years. Current and lifetime psychiatric diagnoses were assessed with the Structured Clinical Interview for Diagnostic and Statistical Manual of Mental Disorders - DSM-IV Axis I and Axis II Disorders and with the Addiction Severity Index-Expanded Version. DSH was assessed with The Deliberate Self-Harm Inventory. Multivariable logistic regression models were used to identify independent correlates of lifetime DSH.
Results:Ninety-three of 526 inmates (17.7%) reported at least 1 lifetime DSH behavior, and 58/93 (62.4%) of those reported a DSH act while in prison. After multivariable adjustment (sensitivity 41.9%, specificity 96.1%, area under the curve = 0.854, 95% confidence interval CI = 0.811–0.897, P < 0.001), DSH was significantly associated with lifetime psychotic disorders (adjusted Odds Ratio aOR = 6.227, 95% CI = 2.183–17.762, P = 0.001), borderline personality disorder (aOR = 6.004, 95% CI = 3.305–10.907, P < 0.001), affective disorders (aOR = 2.856, 95% CI = 1.350–6.039, P = 0.006) and misuse of multiple substances (aOR = 2.024, 95% CI = 1.111–3.687, P = 0.021).
Conclusions:Borderline personality disorder and misuse of multiple substances are established risk factors of DSH, but psychotic and affective disorders were also associated with DSH in male prison inmates. This points to possible DSH-related clinical sub-groups, that bear specific treatment needs.
Euthymia is not always euthymia: Clinical status of bipolar patients after 6 months of clinical remission
- L. Samalin, I. De chazeron, M. Reinares, C. Torrent, C.D.M. Bonnin, D. Hidalgo, A. Murru, I. Pacchiarotti, F. Bellivier, P.M. Llorca, E. Vieta
-
- Journal:
- European Psychiatry / Volume 33 / Issue S1 / March 2016
- Published online by Cambridge University Press:
- 23 March 2020, p. S125
-
- Article
-
- You have access Access
- Export citation
-
Introduction
Most studies selected euthymic patients with bipolar disorder in inter-episodic phase according to clinical remission criteria at least between 1 and 6 months. However, possible differences can exist in the course of clinical symptoms in bipolar patients related to the duration of clinical remission.
ObjectivesThe main aim of this study was to evaluate the clinical status of bipolar patients after 6 months of clinical remission.
MethodsWe performed a cross-sectional study of bipolar outpatients in clinical remission for at least 6 months. Bipolar Depression Rating Scale (BDRS), Young Mania Rating scale, Pittsburgh Sleep Quality Index (PSQI) scale, Visual Analogic Scales (VAS) evaluated cognitive impairment were used to assess residual symptomatology of patients. Multivariate analysis (MANCOVA) was conducted for analysing possible differences between 3 groups of patients according to their duration of clinical remission (< 6 months–1 year, < 1 year–3 years, < 3 years–5 years).
ResultsA total of 525 patients were included into the study. The multivariate analysis indicated a significant effect of the duration of clinical remission on the different residual symptoms (Pillai's trace: F 4.48, P < 0.001). The duration of clinical remission was associated with the significant improvement of the BDRS total score (P = 0.013), the PSQI total score (P < 0.001) and the cognitive VAS total score (P < 0.001)
ConclusionThese results support a possible improvement of residual symptoms according to the duration of clinical remission in bipolar patients. Any definition of euthymia should specify the duration criteria.
Disclosure of interestThe authors have not supplied their declaration of competing interest.
Initial usability and feasibility evaluation of the SIMPLe Smartphone application to monitor and psychoeducate bipolar patients
- D. Hidalgo-Mazzei, M. Reinares, A. Mateu, A. Murru, C.D.M. Bonnín, E. Vieta, F. Colom
-
- Journal:
- European Psychiatry / Volume 33 / Issue S1 / March 2016
- Published online by Cambridge University Press:
- 23 March 2020, p. S122
-
- Article
-
- You have access Access
- Export citation
-
Background
The SIMPLe project was designed with the aim of developing a smartphone application (i.e. app) to monitor and psychoeducate subjects with bipolar disorder through highly personalized messages from both passive and active data. The project was based on a face-to-face group program, which has an increasing scientific evidence of its efficacy and cost-effectiveness reducing bipolar disorder relapses.
AimsAn initial feasibility study was conducted to evaluate the usability and satisfaction of an Android version of the SIMPLe app 1.0.
MethodsThe SIMPLe feasibility study was conducted from March 2015 to June 2015. The participation in the study was offered to a consecutive sample of adult patients diagnosed of bipolar disorder I, II or NOS (not otherwise specified) attending the outpatient mental health clinic of the Hospital Clinic of Barcelona, Spain.
ResultsThe participation in the study was offered to 72 stable bipolar patients. Forty-three subjects were enrolled in the study. Since the day the patients were enrolled in the study, the rate of completed tests was 0.74 per day and 1.13 per week. Nine emergency alerts were received through the application and notified to the reference patients’ psychiatrists. Ninety-five percent of the initial participants remained actively using the app and no relapses were identified during the 3 months of the study.
ConclusionThese preliminary results suggest a high feasibility of the SIMPLE app based on the rates of tasks completed and retention.
Disclosure of interestThe authors have not supplied their declaration of competing interest.
Determinants of Functioning in Euthymic Patients with Bipolar Disorder: A Structural Equation Modelling Approach
- L. Samalin, L. Boyer, A. Murru, I. Pacchiarotti, M. Reinares, C.M. Bonnin, C. Torrent, V. Norma, P. Corinna, I. de Chazeron, M. Boucekine, P.A. Geoffroy, F. Bellivier, P.M. Llorca, E. Vieta
-
- Journal:
- European Psychiatry / Volume 41 / Issue S1 / April 2017
- Published online by Cambridge University Press:
- 23 March 2020, p. S77
-
- Article
-
- You have access Access
- Export citation
-
Background
Euthymic patients with bipolar disorder (BD) experience residual symptoms. Interestingly, residual symptoms appear to impact the natural course of BD and represent potential predictors of recurrence and functional impairment.
ObjectivesThe study aimed to analyse the relationship between residual depressive symptoms, sleep disturbances and cognitive impairment as determinants of psychosocial functioning in a large sample of euthymic BD patients.
MethodsWe performed a cross-sectional study of 468 BD outpatients in clinical remission for at least 6 months. Bipolar Depression Rating Scale (BDRS), Pittsburgh Sleep Quality Index (PSQI) scale, Visual Analogic Scales (VAS) evaluated cognitive impairment and functioning assessment short test were used to assess residual symptomatology and functioning of patients. We evaluated functioning with. Structural equation modelling (SEM) was used to describe the relationships among the residual depressive symptoms, sleep disturbances, perceived cognitive performance and functioning.
ResultsSEM showed good fit. This model revealed that residual depressive symptoms (path coefficient = 0.37) and perceived cognitive performance (path coefficient = 0.27) were the most important features significantly related to psychosocial functioning. Sleep disturbances were indirectly associated with functioning via residual depressive symptoms and perceived cognitive performance (path coefficient = 0.23).
ConclusionsThis study contributes to a better understanding of the determinants of psychosocial functioning during the interepisodic periods of BD patients. These findings should have implications for the improvement of functioning of BD patients in a personalized approach to treatment.
Disclosure of interestCOI: Dr. Samalin reports personal fees and nonfinancial support from Astra-Zeneca, Bristol Myers Squibb, Janssen, Lundbeck, and Otsuka.
The authors L. Boyer, A. Murru, I. Pacchiarotti, M. Reinares, C.M. Bonnin, C. Torrent, V. Norma, P. Corinna, I. de Chazeron, M. Boucekine, P.A. Geoffroy, F. Bellivier, P.M. Llorca, E. Vieta have have not supplied their declaration of competing interest.
A 12-month prospective study on the time to hospitalization and clinical management of a cohort of bipolar type I and schizoaffective bipolar patients
- Andrea Murru, Norma Verdolini, Gerard Anmella, Isabella Pacchiarotti, Ludovic Samalin, Alberto Aedo, Juan Undurraga, José M. Goikolea, Benedikt L Amann, Andre F. Carvalho, Eduard Vieta
-
- Journal:
- European Psychiatry / Volume 61 / September 2019
- Published online by Cambridge University Press:
- 01 January 2020, pp. 1-8
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Background.
Schizoaffective disorder, bipolar type (SAD) and bipolar disorder I (BD) present a large clinical overlap. In a 1-year follow-up, we aimed to evaluate days to hospitalization (DTH) and predictors of relapse in a SAD-BD cohort of patients.
Methods.A 1–year, prospective, naturalistic cohort study considering DTH as primary outcome and incidence of direct and indirect measures of psychopathological compensation as secondary outcomes. Kaplan-Meyer survival analysis with Log-rank Mantel-Cox test compared BD/SAD subgroups as to DTH. After bivariate analyses, Cox regression was performed to assess covariates possibly associated with DTH in diagnostic subgroups.
Results.Of 836 screened patients, 437 were finally included (SAD = 105; BD = 332). Relapse rates in the SAD sample was n = 26 (24.8%) vs. n = 41 (12.3%) in the BD sample (p = 0.002). Mean ± SD DTH were 312.16 ± 10.6 (SAD) vs. 337.62 ± 4.4 (BD) days (p = 0.002). Patients with relapses showed more frequent suicide acts, violent behaviors, and changes in pharmacological treatments (all p < 0.0005) in comparison to patients without relapse. Patients without relapses had significantly higher mean number of treatments at T0 (p = 0.010). Cox regression model relating the association between diagnosis and DTH revealed that BD had higher rates of suicide attempts (HR = 13.0, 95%CI = 4.0–42.0, p < 0.0005), whereas SAD had higher rates of violent behavior during psychotic episodes (HR = 12.0, 95%CI =.3.3-43.5, p > 0.0005).
Conclusions.SAD patients relapse earlier with higher hospitalization rates and violent behavior during psychotic episodes whereas bipolar patients have more suicide attempts. Psychiatric/psychological follow-up visits may delay hospitalizations by closely monitoring symptoms of self- and hetero-aggression.








